Types of Arthritis
There are many types of arthritis out there, but did you know that there are over one hundred forms of it?
It seems to be growing in numbers each year, making it the most common illness in The United States of America.
That’s pretty shocking, isn’t it? It’s hard to believe that there can be so many different types of this condition, but there are.
Each form of arthritis will affect a person in such different ways, even twisting the hands and feet with some conditions.
Some types of arthritis will also cause a person to lose complete control of range of motion! Today, we are going to be taking a look at a few forms of arthritis.
Osteoarthritis
This type of arthritis affects millions of people worldwide but is more common in The United States.
A lot of the times, this type of illness is called degenerative disk disease and what this is, is merely the wear and tear of a person’s joints which does sound quite scary, I know.
The most common symptom of this form of arthritis is extreme stiffness, especially after sitting for long periods of time or when a person first rises in the mornings.
This is because the joints have not been moving and active during the night. The treatment for such an illness is to exercise, as this keeps the joints healthy and robust, as well the usage of various forms of prescription medications.
Lupus
Many people wouldn’t think that Lupus is a form of arthritis, but in fact, it is. Lupus is a long-lasting autoimmune illness which will affect different portions of a person’s body, including the joints, of course, the kidneys, as well other organs. It can also affect the skin, bloodstream, as well the brain.
The symptoms of this illness can include feeling fatigued out, rashes, joint pain, as well photosensitivity.
The treatment for such illness consists of a combination of specific medications, as well lifestyle changes.
Keep in mind that these changes will not cure Lupus, but it will help to manage and deal with the illness itself.
Rheumatoid Arthritis
Now, this form of arthritis is very serious, although all forms of arthritis are quite serious, but not in the way that rheumatoid arthritis is.
This is an autoimmune illness which can cause a person’s body to twist and form in very odd ways. Some of the most common ways will be knotty, twisty fingers and toes that you see in a lot of older people. Keep in mind that along with the common inflammation and pain, a person can also feel a loss of appetite, fatigue, and even a low-grade fever.
Rheumatoid arthritis is a severe condition and remember; there isn’t a cure for this kind of arthritis.
A person can only prevent the symptoms from getting worse through various medications and forms of exercise.
Chronic Fatigue Syndrome
What makes this type of arthritis so strange is the fact that it’s a complete state of profound fatigue which lasts six months or even longer.
It’s not improved by bed rest, and this condition could very well get worse with mental or physical activity!
This type of arthritic symptom deeply interferes with a person’s daily events, as well work.
The cause of chronic fatigue syndrome is still unknown as to why it happens and some of the symptoms including the following.
If you are a sufferer of chronic fatigue syndrome, you will tend to experience general weakness, muscles, and joints which ache, exhaustion, tender lymph nodes, difficulty sleeping, headaches, experiencing dizziness, as well experiencing a low-grade fever. Once again, there is no cure for this type of arthritis, but it can be treated with prescription medications.
Gout
This is a form of an anti-inflammatory illness which will develop in some individuals that have high levels of uric acid inside the bloodstream.
It’s more than likely to affect men than women, and this condition occurs in four percent of adult Americans.
One of the most common symptoms of gout is extreme pain and swelling in the big toe, but keep in mind that this condition can also show up in the knees and ankles as well. One way to treat gout is to make sure that you always keep your uric acids levels down, as well taking prescription medications to take the severity of gout away.
Arthritis Myths
There are so many different types of myths out there when it comes to arthritis, how to heal and cope with it, what causes it and so on.
The actual list of arthritis myths could go on for quite the long time. A myth is a kind of an opinion that has a lot of popularity.
There could be some, remember that word some.
There could be some truth to it and then again, the whole myth could not hold an ounce of truth to it.
That’s the mystery of it all and today; we are going to be taking a look at some of the most strange and common myths out there circulating about arthritis.
What Are Some of The Myths Circulating About Arthritis?
- Popping one’s knuckles will cause arthritis, and that is probably one of the most common myths out there relating to arthritis! Popping your fingers will not lead to arthritis, maybe just an annoying sound around others, but no this type of behavioral pattern will most probably not lead to forms of arthritis.
- It’s a leading myth of arthritis that only elder individuals will get this condition, which is entirely incorrect! There have been accounts of teenagers developing various forms of arthritis! Remember, a child can be born with crippling arthritis from the time it takes its first breath.
- Some types of arthritis are hereditary and cannot be reversed. So, not only elder persons can develop arthritis. Although, it is prevalent for women aged fifty or more to develop arthritis, so this bracket will be placed at a higher risk because of the weakness and wearing out of the bones, but there have been cases where younger people can develop arthritis.
- It’s been said that arthritis cannot be prevented and that is most definitely false. Keep in mind that although a person is male or female and nature cannot alter that, there are things that a person can do to prevent the severity of developing various forms of arthritis. Such activities include maintaining a proper diet, exercising on a regular basis, wearing the appropriate gear during any physical sport, not smoking, and so on. We must remember that we all only get one set of bones throughout our lives, so we need to be profound on taking proper care of what we have to preserve as much health in our bones as we possibly can.
- It has also been stated that once a person is identified with arthritis, there isn’t a lot he or she will be able to do about that fact and once again, that is false. Why would this myth be false? Well, keep in mind that there isn’t a complete treatment for arthritis just yet, but there are a lot of great medications, herbal supplements, and natural healing practices that a person can undergo to better cope and deal with the irritation of arthritis.
- Some people will even state that once a person has been diagnosed with arthritis, they should wait and see if the symptoms go away naturally, which is the absolute wrong thing to do! Did you know that early attention, as well handling can preserve more than just a person’s joints? That’s right! There are some forms of arthritis which can source injury to the heart, as well other organs in a person’s body. It’s vital, and we mean, crucial that you know exactly what category of arthritis that you have to obtain proper treatment of whichever type you have. Most people do not see this, but there are over one hundred types of arthritis and if you do not know which type you have, how would you be able to treat it? You must know exactly what form of arthritis you have because, in the long run, it could indeed save your life.
- Some people will think that their diet has nothing to do with arthritis, but in fact, it does. Did you know that people who have arthritis will nine times out of ten, develop diabetes?
- This is why obtaining a proper diet is essential in preventing the severity of arthritis! Fish oil, Mediterranean foods, and Omega-3 Fatty Acids are vital to consume in your diet because these types of elements work in the body to reduce inflammation throughout the joints and muscles.
Rheumatoid arthritis – causes, symptoms, diagnosis, treatment, pathology
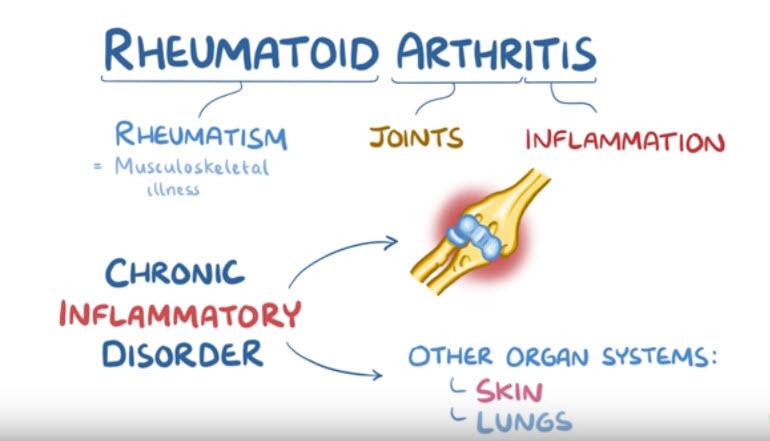
In rheumatoid arthritis, “arthr-“ refers to joints, “-itis” means inflammation, and “rheumatoid” comes from rheumatism, which more broadly refers to a musculoskeletal illness.
So, rheumatoid arthritis is a chronic, inflammatory disorder that mostly affects the joints, but can also involve other organ systems like the skin and lungs as well.
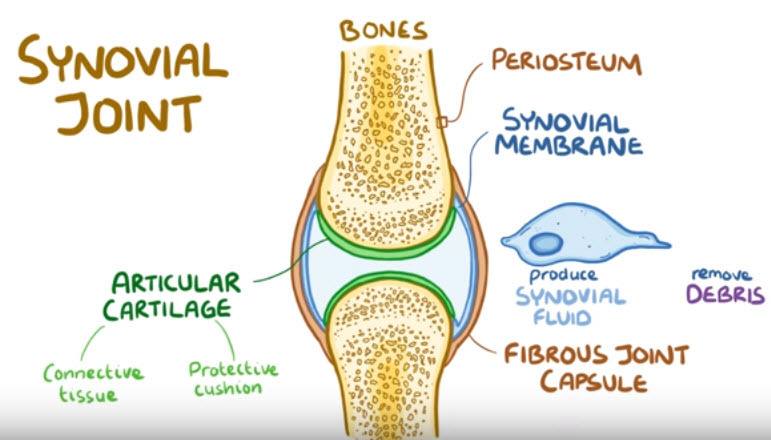
A healthy joint typically has two bones covered with articular cartilage at the ends.
Articular cartilage is a type of connective tissue that acts like a protective cushion – a lubricated surface for bones to smoothly glide against.
One type of joint, like the knee joint is called a synovial joint.
A synovial joint connects two bones with a fibrous joint capsule that is continuous with the periosteum or outer layer of both bones.
The fibrous capsule is lined with a synovial membrane that has cells that produce synovial fluid and remove debris.
The synovial fluid is normally a viscous fluid like the jelly-like part of a chicken egg and it helps lubricate the joint.
To help serve these synovial cells, the synovial membrane also has blood vessels and lymphatics running through it.
Together, the synovial membrane and the articular cartilage form the inner lining of the joint space.
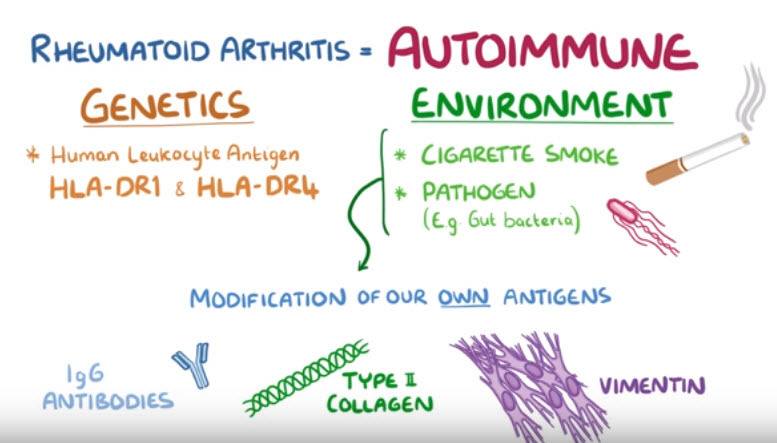
Rheumatoid arthritis is an autoimmune process that is typically triggered by an interaction between a genetic factor and the environment.
For example, a person with a certain gene for an immune protein like human leukocyte antigen, or HLA- DR1 and HLA–DR4, might develop rheumatoid arthritis after getting exposed to something in the environment like cigarette smoke or a specific pathogen like a bacteria that lives in the intestines.
These environmental factors can cause modification of our own antigens, such as IgG antibodies or other proteins like type II collagen or vimentin.
Τype II collagen and vimentin can get modified through a process called citrullination.
That’s when the amino acid arginine found in these proteins is converted into another amino acid, citrulline.
Meanwhile, due to the susceptibility genes HLA- DR1 and HLA–DR4, immune cells sometimes are not “clever” enough, so they get confused by these changes and they no longer recognize these proteins as self-antigens.
The antigens get picked up by antigen- presenting cells, and get carried to the lymph nodes to activate CD4+ T-helper cells.
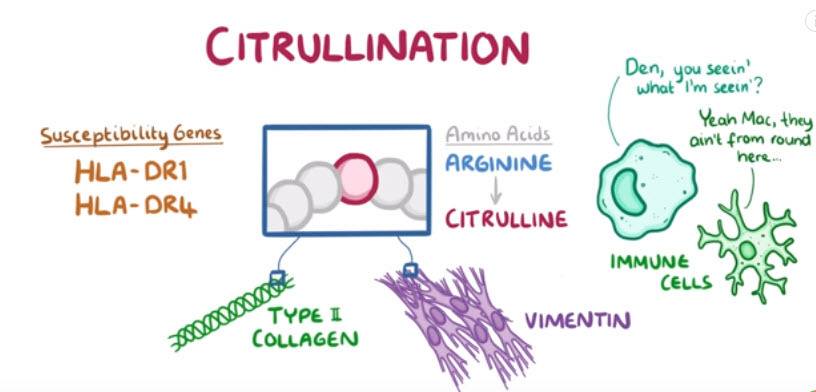
T-helper cells stimulate the nearby B- cells to start proliferating and differentiate into plasma cells, which produce specific autoantibodies against these self- antigens.
In rheumatoid arthritis, T- helper cells and antibodies enter the circulation and reach the joints.
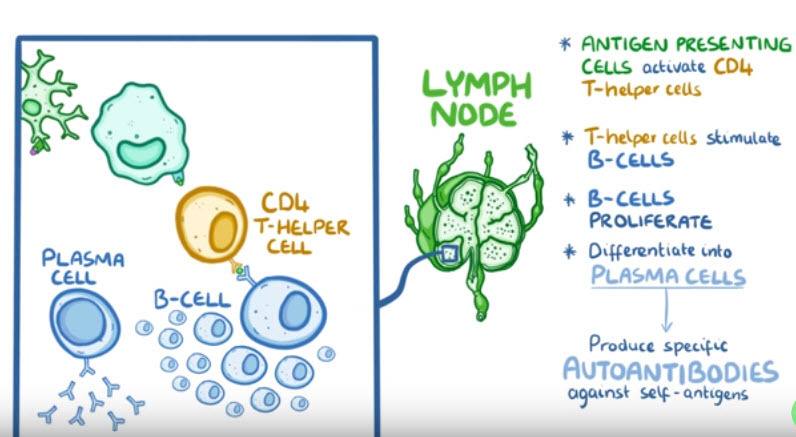
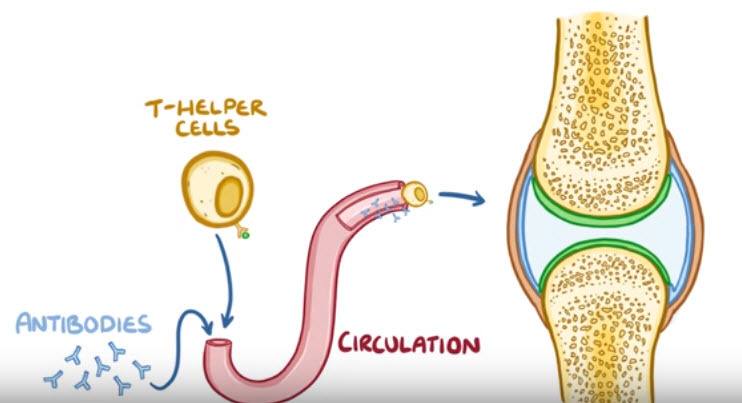
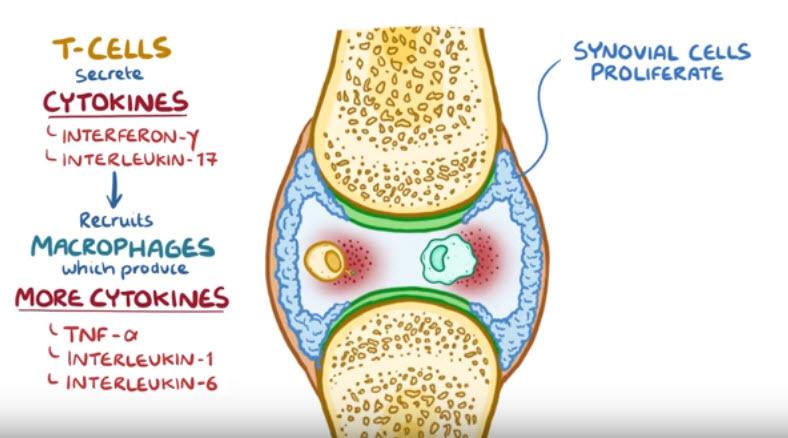
Once there, T- cells secrete cytokines like interferon- γ and interleukin- 17, to recruit more inflammatory cells like macrophages, into the joint space.
Macrophages will also produce inflammatory cytokines, like tumor necrosis factor, or TNF- α, interleukin- 1 and interleukin- 6, which together with the T-cell’s cytokines, stimulate synovial cells to proliferate.
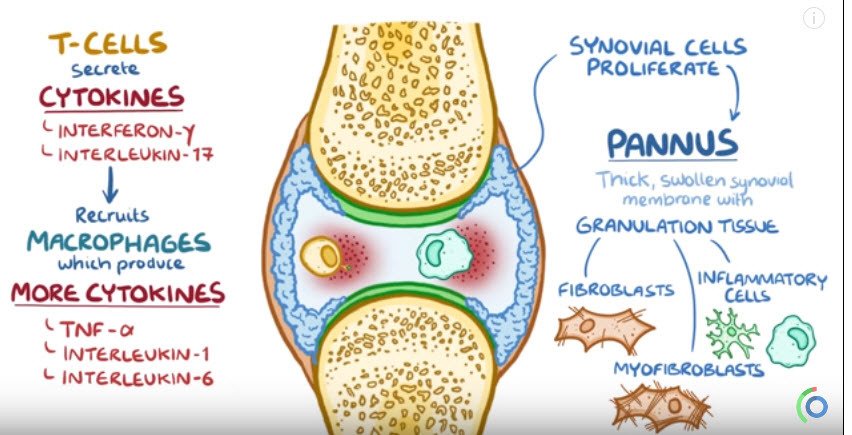
The increase in synovial cells and immune cells creates a pannus, which is a thick, swollen synovial membrane with granulation or scar tissue, made up of fibroblasts, myofibroblasts and inflammatory cells.
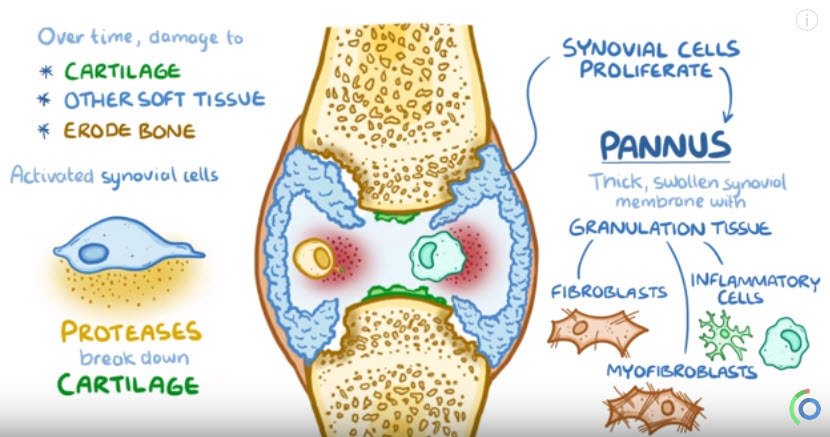
Over time, the pannus can damage cartilage and other soft tissues and also erode bone.
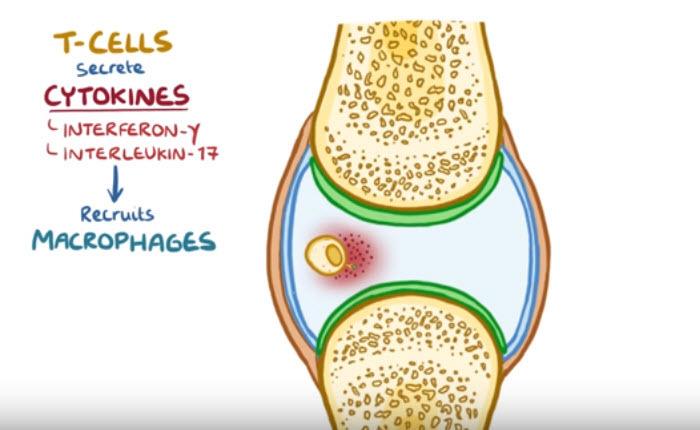
Activated synovial cells also secrete proteases which break down the proteins in the articular cartilage.
Without the protective cartilage, the underlying bones are exposed and can directly rub against one another.
In addition, inflammatory cytokines increase a protein on the surface of T- cells, known as RANKL or receptor activator of nuclear factor kappa-B ligand. RANKL allows the T-cells to bind RANK, a protein on the surface of osteoclasts, to get them to start breaking down bone.
Meanwhile, antibodies also enter the joint space.
One antibody is called rheumatoid factor, or RF, which is an IgM antibody that targets the constant Fc domain of altered IgG antibodies.
Another antibody is anti-cyclic citrullinated peptide antibody, or CCP, which targets citrullinated proteins.
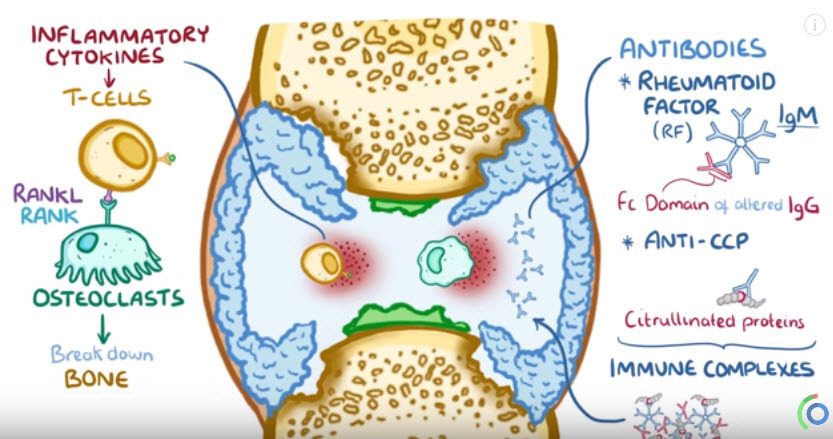
When these antibodies bind to their targets, they form immune complexes which accumulate in the synovial fluid.
There, they activate the complement system, a family of 9 small proteins that work in an enzymatic cascade to promote joint inflammation and injury.
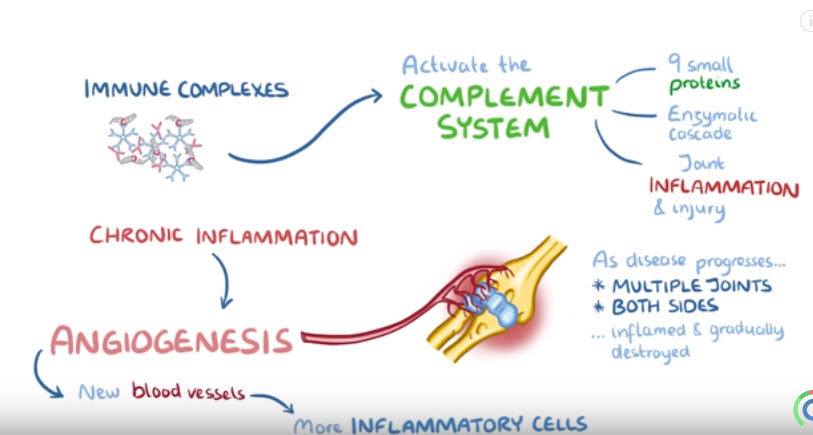
Finally the chronic inflammation causes angiogenesis, or the formation of new blood vessels around the joint, which allows even more inflammatory cells to arrive.
As the disease progresses, multiple joints on both sides of the body get inflamed and gradually destroyed.
But these inflammatory cytokines don’t just stay within the tight joint space.
Instead, they escape through the bloodstream and reach multiple organ systems causing extra-articular problems, meaning problems beyond the joint space.
For example, interleukin-1 or -6 travel to the brain, where they act as pyrogens, inducing fever.
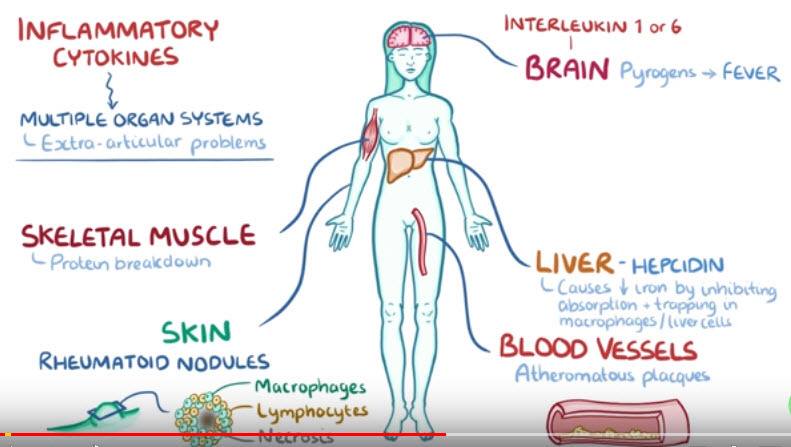 In skeletal muscle, they promote protein breakdown and in the skin, as well as in many visceral organs, they lead to the formation of rheumatoid nodules, which are round- shaped collections of macrophages and lymphocytes with a central area of necrosis, or tissue death.
In skeletal muscle, they promote protein breakdown and in the skin, as well as in many visceral organs, they lead to the formation of rheumatoid nodules, which are round- shaped collections of macrophages and lymphocytes with a central area of necrosis, or tissue death.
Blood vessels can also be affected.
Their walls get inflamed, resulting in various forms of vasculitis and make them prone to developing atheromatous or fibrofatty plaques.
In response to inflammatory cytokines, the liver also starts producing high amounts of hepcidin, a protein that decreases serum iron levels by inhibiting its absorption by the gut and trapping it into macrophages or liver cells.
Meanwhile, within the lung interstitium, fibroblasts get activated and proliferate, causing fibrotic or scar tissue that makes it harder for the alveolar gas exchange, while also the pleural cavities surrounding the lungs can get inflamed, filling up with fluid, known as pleural effusion, and this can sometimes mess with lung expansion.
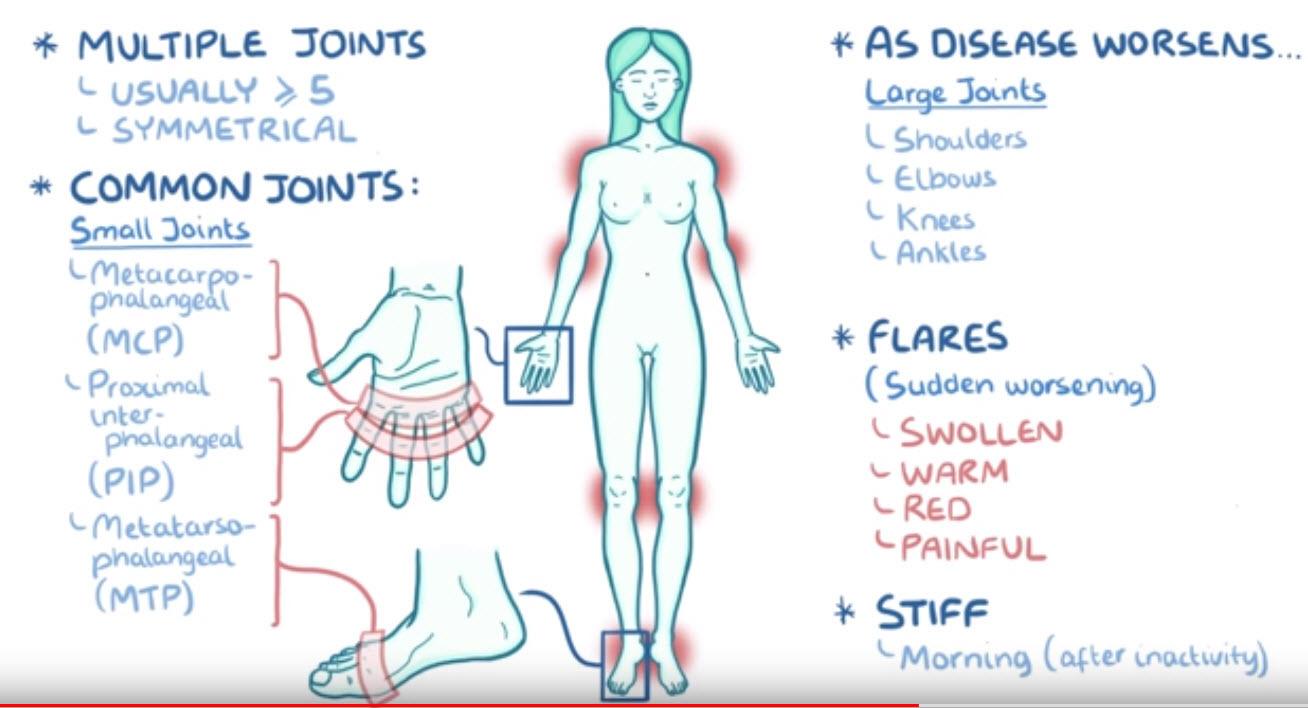
Rheumatoid arthritis typically involve multiple joints, usually five or more, symmetrically, meaning the same joint groups on both sides of the body, like both hands for instance. Commonly affected joints are the small joints like metacarpophalangeal and proximal interphalangeal joints of the hands, and the metatarsophalangeal joints of the feet.
As the disease worsens, it can start to affect large joints like the shoulders, elbows, knees and ankles.
During “flares” or sudden worsening of the disease, the affected joints get extremely swollen, warm, red, and painful.
Over time, they become stiff, especially in the morning or after being inactive for a prolonged period of time.
People with rheumatoid arthritis may develop specific deformities, usually of the metacarpophalangeal joints in the hand, such as ulnar deviation of the fingers.
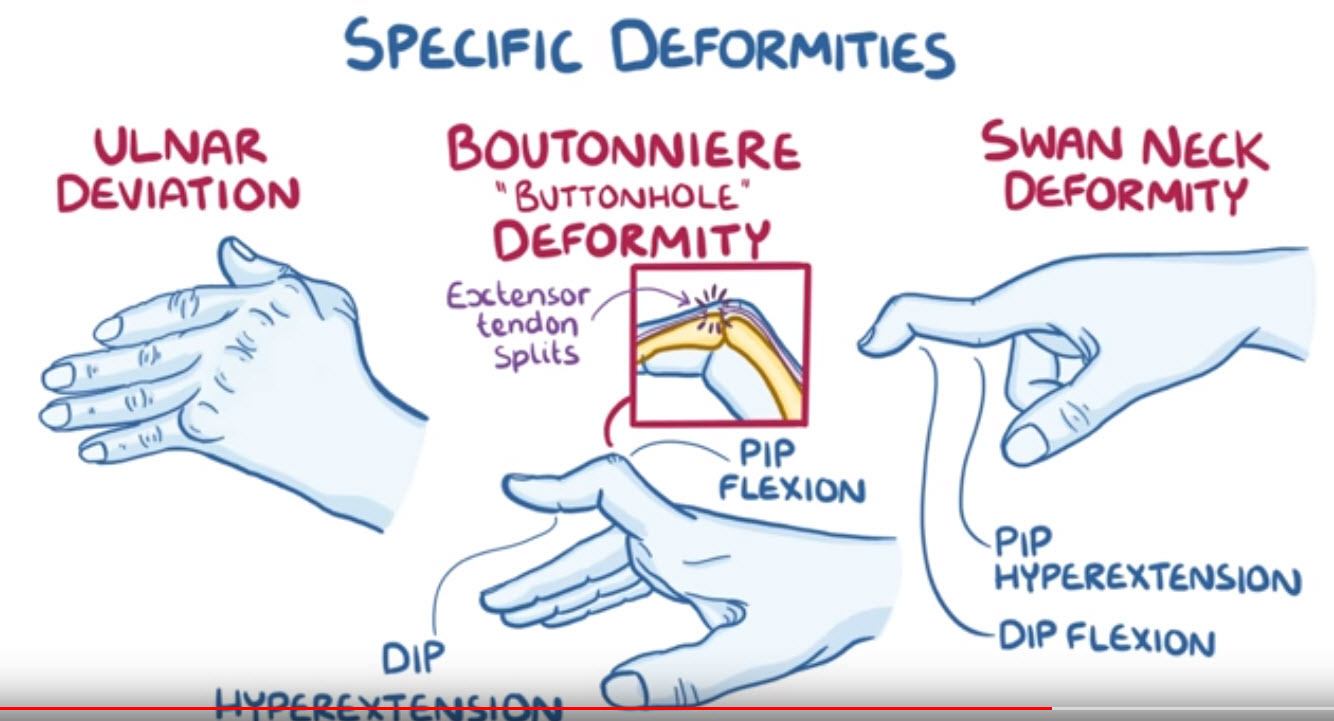
Deformities are also common in the interphalangeal joints, such as the so- called boutonniere or buttonhole deformity.
This occurs when the extensor tendon in the back of the finger splits and the head of the proximal phalanges pokes through like a button through a buttonhole, causing flexion of the proximal interphalangeal joint and hyperextension of distal interphalangeal joint.
Another finger deformity is the swan neck deformity, which is the opposite, so there’s hyperextension of the proximal interphalangeal joint and flexion of the distal interphalangeal joint.
Now, in the knee joint, a one-way value can form, with fluid from the swollen knee filling the semi-membranous bursa.
When that happens, the synovial sac can get so swollen that it bulges posteriorly into the popliteal fossa, creating a synovial fluid-filled cyst, called a Baker or popliteal cyst.
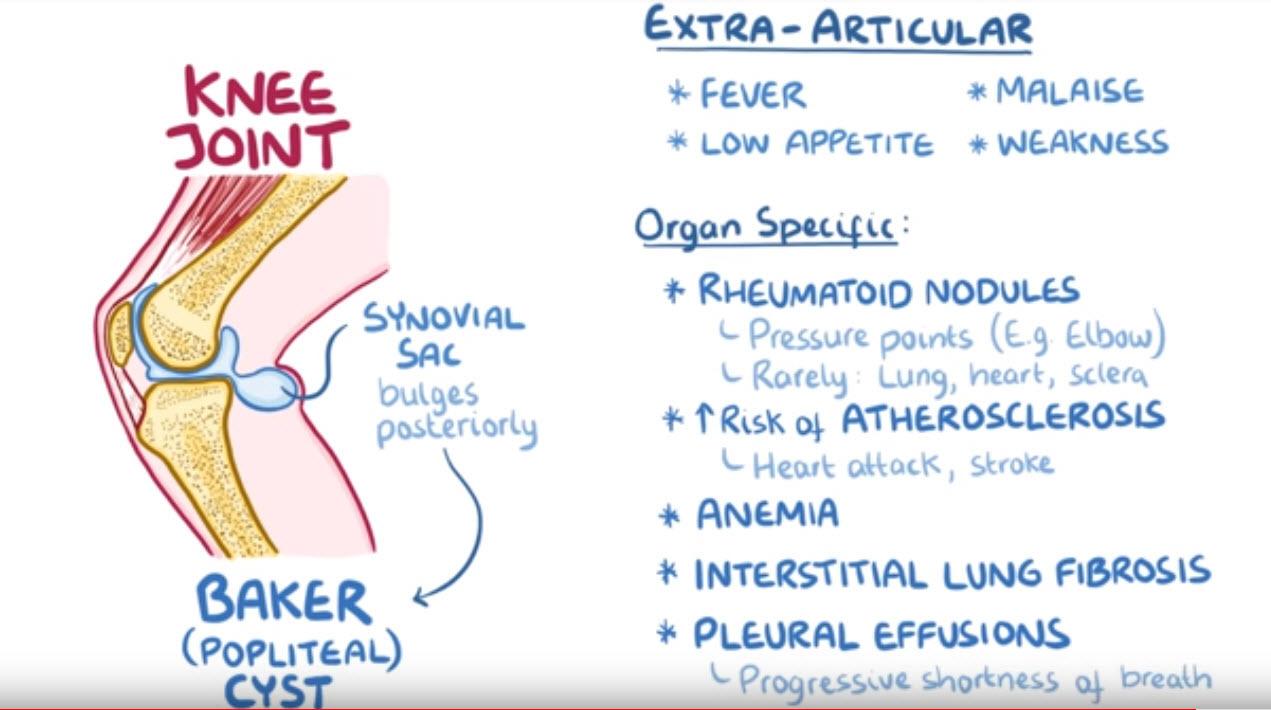
Now, extra- articular manifestations include non-specific symptoms of inflammation, such as fever, low appetite, malaise or muscle weakness, and organ- specific, manifistations include rheumatoid nodules or firm bumps of tissue, and these most commonly in the skin around pressure points, such as the elbows.
More rarely, in the lungs, the heart, or the sclera of the eye.
There’s also an increased risk of atherosclerosis and therefore, heart attack or stroke.
There’s also anemia, interstitial lung fibrosis and pleural effusions, which can present as progressive shortness of breath.
One particularly serious condition that’s associated with rheumatoid arthritis is Felty syndrome which is a triad of rheumatoid arthritis, splenomegaly, and granulocytopenia, and it can lead to life-threatening infections.
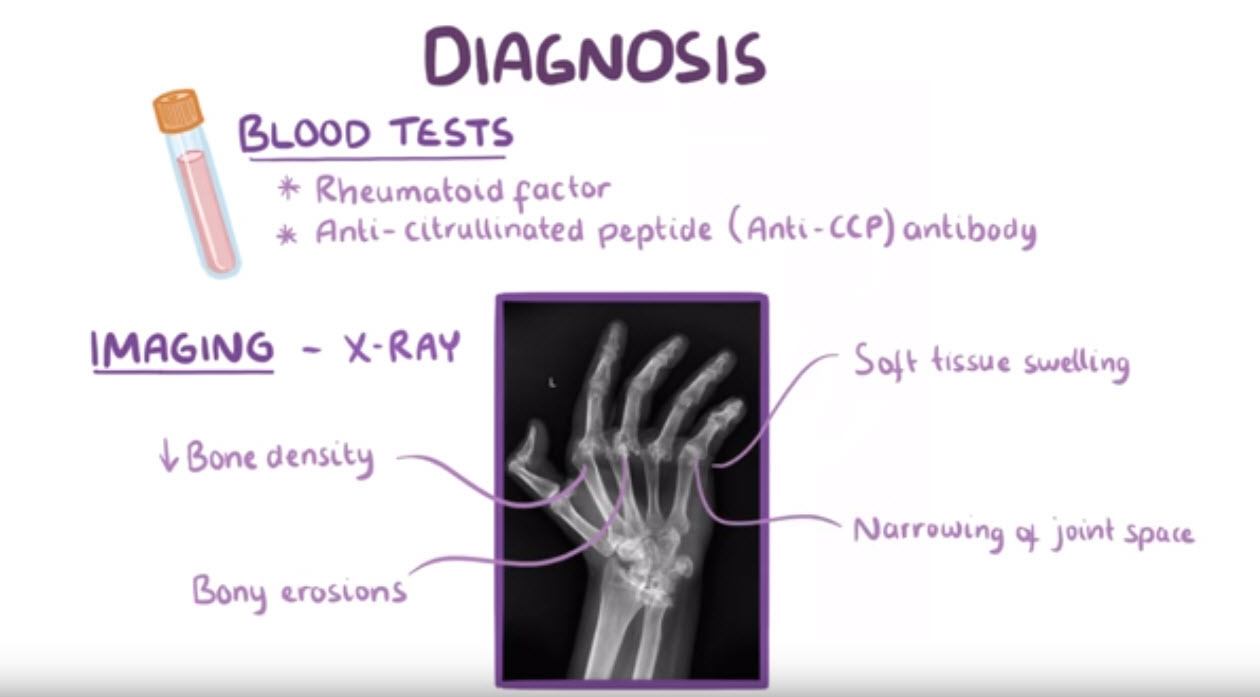
Diagnosis of rheumatoid arthritis usually involves confirmatory blood tests, like looking for the presence of rheumatoid factor and anti-citrullinated peptide antibody. Additionally, imaging studies, such as X- ray, usually reveal decreased bone density around affected joints, soft tissue swelling, narrowing of the joint space, and bony erosions.
The long term management of rheumatoid arthritis is use of disease-modifying anti-rheumatic medications like methotrexate, hydroxychloroquine, sulfasalazine, and which can help to suppress the inflammation. In addition, there are a variety of medications called biologic response modifiers or biologics. Some biologics, such as abatacept, work by suppressing the activity of T cells, or others, such as rituximab suppress B cells.
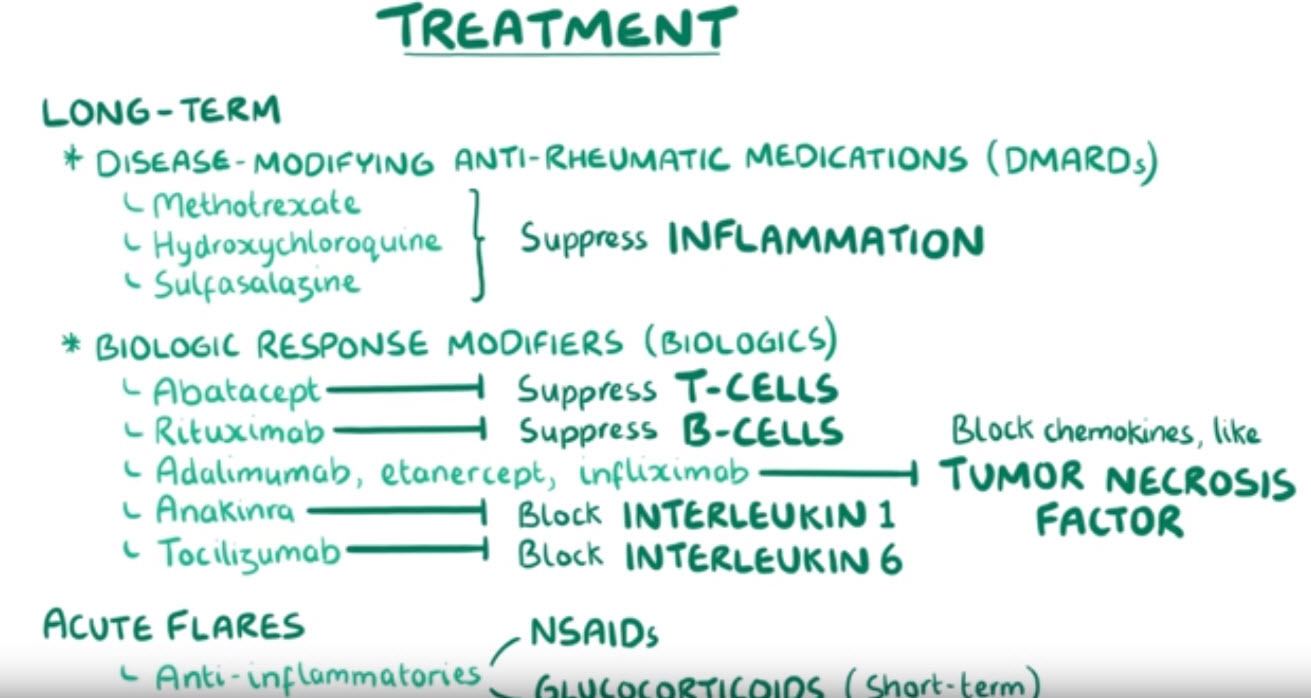
There are also biologics such as adalimumab, etanercept, and infliximab, that block various chemokines like tumor necrosis factor.
Anakinra blocks interleukin 1 which is blocked by, and tocilizumab blocks interleukin 6.
Treatment of acute flares can be done with anti- inflammatory medications like NSAIDS as well as short term use of glucocorticoids.
To conclude, rheumatoid arthritis is a systemic inflammatory disorder of autoimmune origin that is primarily characterized by progressive, symmetric joint destruction, especially in the wrists and fingers, but may also affect other joints and many organs, such as the skin, heart, blood vessels and lungs.
It’s marked by elevated rheumatoid factor and anti- cyclic citrullinated peptide antibodies..
As found on Youtube
