
Allergies and Headaches – What Is the Connection?
The American Academy of Allergy, Asthma and Immunology (AAAAI) reports that somewhere around ” 80% of the North American population has headaches, with 50% experiencing at least one headache per month.” Roughly 1 in 6 or 7 people in America experience a minimum of one headache per day.
Similar figures are reported in the United Kingdom, Asia, Australia, Canada and other nations.
It is interesting to note that AAAAI reports headaches rise dramatically in the second decade of life for humans, and then start to drop off in regularity and severity after the age of 40 or 50. In many cases, your headaches may be tied to some type of allergy you may have, whether you are aware of your allergic condition or not.
In the case of hay fever (rhinitis), headaches might be the product of sinus pressure which accompanies that seasonal allergy.
Different allergies cause different levels of headache pain, and sometimes lead to no headaches at all.

Headache
Sinusitis
Dr. Jonathan Field is the director of the Allergy and Asthma Clinic at the New York University School of Medicine/Bellevue Medical Center in New York City.
He says that the ” most common cause of the migraine is allergenic sinusitis.”
This happens when someone is exposed to an allergen like animal hair, pollen or dust, which causes an allergic response in that person.
Other people may not be allergic to those airborne contaminants.
However, an allergic person immediately experiences a swelling in the sinuses.
This often causes mild headaches or intense migraines. In the case of migraines, the nerves in the brain respond to a change in the sinus pressure.
Typical migraine symptoms such as a headache, nausea, vomiting, dizziness and an intolerance to light or sound are then experienced.
Sometimes sinus pressure due to allergies doesn’t cause a severe migraine.
However, the pressure that happens can still lead to minor headache symptoms which are aggravating, frustrating and painful.
Histamines
Your body produces a chemical called histamine and it is released as a response to an allergic reaction.
When your histamine levels are very high, you can suffer a swelling of the sinuses, headaches, itchy eyes and other symptoms typically identified as accompanying seasonal allergies.
Because of this connection, a lot of hay fever and other seasonal allergy medications contain antihistamines.
They fight the swelling of your sinuses and other responses triggered in your immune system when an allergen is present.
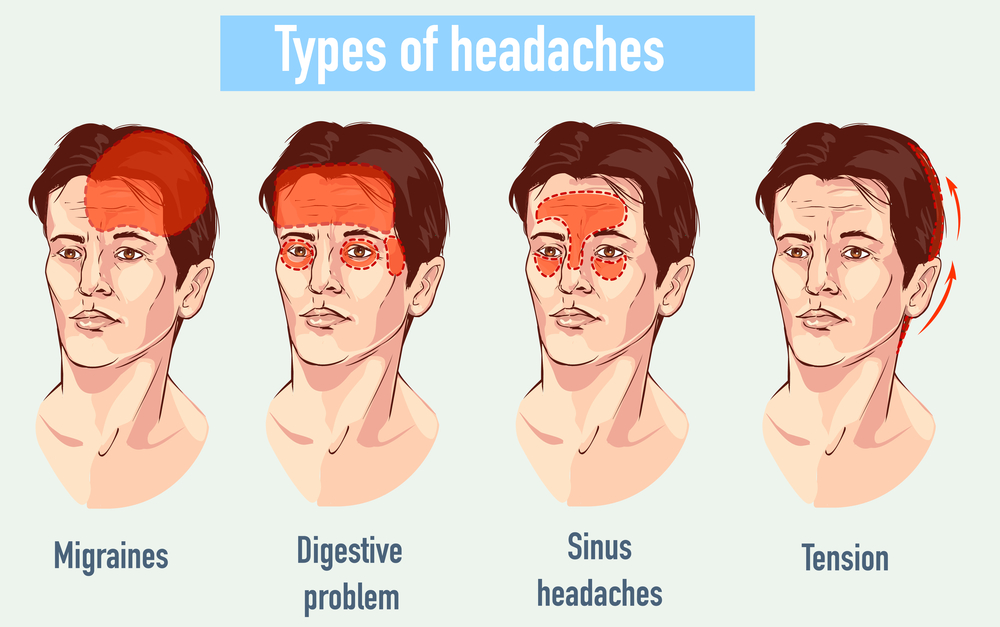
headaches 4 type on different area of patient head.
Sinus Headache
Symptoms
The sinus cavities are hollow air spaces with openings into the nose to allow the exchange of air and mucus.
They are located inside each cheekbone, behind the eyes, behind the bridge of the nose and in the forehead.
Secretions from the sinus cavities normally drain into the nose.
Sinus headaches and pain occur when the sinuses are swollen and their openings into the nasal passages are obstructed, stopping normal drainage and causing pressure to build up.
Often the pain is localized over the affected sinus, perhaps causing facial pain rather than a headache.
For example, if the maxillary sinus in the cheeks is obstructed, your cheeks may be tender to the touch and pain may radiate to your jaw and teeth.
Obstruction in other sinuses can cause pain on the top of your head or elsewhere.
Sinus pain can be dull to intense; it often begins in the morning and becomes less intense after you move from lying flat to sitting or standing in an upright position.
Similar pain can also be caused by severe nasal congestion, particularly if you have a deviated septum or a septal “spur” from a previous nasal injury. Such “headaches” or facial pain can involve one side only.
Management and Treatment
The first approach in managing sinus headaches is to avoid the allergens that trigger them.
Outdoor exposure:
- Stay indoors as much as possible when common triggers, such as high pollen counts, are at their peak, usually during the midmorning and early evening, and when wind is blowing pollens around.
- Avoid using window fans that can draw pollens and molds into the house.
- Wear glasses or sunglasses when outdoors to minimize the amount of pollen getting into your eyes, as this can cause your sinuses to flare up.
Indoor exposure:
- Keep windows closed, and use air conditioning in your car and home. Air conditioning units should be kept clean.
- Reduce exposure to dust mites, especially in the bedroom. Use “mite-proof” covers for pillows, comforters and duvets, and mattresses and box springs.
- To limit exposure to mold, keep the humidity in your home low (between 30 and 50 percent) and clean your bathrooms, kitchen and basement regularly. Use a dehumidifier, especially in the basement and in other damp, humid places, and empty and clean it often. If mold is visible, clean it with detergent and a 5 percent bleach solution as directed by an allergist.
- Clean floors with a damp rag or mop, rather than dry-dusting or sweeping.
Exposure to pets:
- Wash your hands immediately after petting any animals. Wash your clothes after visiting friends with pets.
- If you are allergic to a household pet, keep it out of your home as much as possible. If the pet must be inside, keep it out of the bedroom so you are not directly exposed to animal allergens while you sleep.
- Close the air ducts to your bedroom if you have forced-air or central heating or cooling. Replace carpeting with hardwood, tile or linoleum, all of which are easier to keep dander-free. Placing an air purifier in the bedroom may also help.
Many allergens that trigger sinus headaches are airborne, so you can’t always avoid them. Discuss your symptoms with your allergist to determine which treatment options are right for you.
Another common cause of sinus headaches is allergic rhinitis (hay fever).
Both prescription and nonprescription (over-the-counter, or OTC) oral medications — antihistamines, decongestants and corticosteroids — are used to treat it.
- Antihistamines. These block the effects of histamine, a chemical produced by the body in response to allergens. Histamine is responsible for the symptoms of allergic rhinitis, including sneezing, itchy eyes and an itchy, runny nose. First-generation OTC antihistamines available in the United States can cause drowsiness, and regularly taking them can lead to a feeling of constant sluggishness, affecting learning, memory and performance. Newer antihistamines — such as Claritin (loratadine) and Zyrtec (cetirizine), both OTC, and Clarinex (desloratadine), Allegra (fexofenadine) and Xyzal (levocetirizine), available by prescription — are designed to minimize drowsiness while still blocking the effects of histamine.
- Oral and nasal decongestants. Found in many OTC and prescription medications, these may be the treatment of choice for the nasal congestion that causes a sinus headache. Decongestants help relieve the stuffiness and pressure caused by swollen nasal tissue.
- Intranasal corticosteroids. This is the single most effective drug class for treating allergic rhinitis. These medications can significantly reduce nasal congestion as well as sneezing, itching and a runny nose.
Other treatments and medications include:
- Allergy shots (immunotherapy). Allergen immunotherapy, or allergy shots, may be recommended for people who don’t respond well to treatment with medications, experience side effects from medications, have allergen exposure that is unavoidable or desire a more permanent solution to their allergy problem.
- Nasal cromolyn. Nasal cromolyn is a nasal spray that blocks the body’s release of allergy-causing substances. Nasal cromolyn can help to prevent allergic nasal reactions if taken prior to an allergen exposure. It does not work in all patients.
- Pain relievers. Mild OTC pain relievers such as Tylenol (acetaminophen) or Advil (ibuprofen) may provide short-term relief for sinus headache pain.
At-home treatments
- Apply a warm, moist washcloth to your face several times a day.
- Drink plenty of fluids to thin the mucus.
- Inhale steam two to four times per day (for example, while sitting in the bathroom with the shower running).
- Spray the nose with nasal saline several times per day.
- Use a neti pot to flush the sinuses.
Sources:
http://www.everydayhealth.com/headache-migraine/migraines-from-allergies.aspx
http://acaai.org/allergies/symptoms/allergy-headaches

